Mohd Syukri1*, Dewi Masyitah1, Mashudi1, Lailatul Fadilah2
1. Department of Nursing, Health Polytechnic, Ministry of Health Jambi, Indonesia
2. Department of Nursing, Health Polytechnic, Ministry of Health Banten, Indonesia
* Corresponding author: Mohd Syukri, Jl. Dr. Tazar, Buluran Kenali, Kec. Telanaipura, Kota Jambi, Jambi 36361, Indonesia, Orcid: https://orcid.org/0000-0003-2061-5531
Email: syukrimuh290@gmail.com
Cite this article
ABSTRACT
Introduction: Along with increasing age, there will also be an increasing tendency to get sick and have physical limitations (disabilities) due to a drastic decline in physical abilities. These conditions are the leading cause of high mortality and morbidity in the elderly, especially during the Covid-19 pandemic. The current study aims to analyze the relationship between psychosocial status and the quality of life of the elderly with osteoarthritis during the Covid-19 pandemic.
Materials and Methods: This cross-sectional study was located at a nursing home in Jambi, involving 351 randomly selected participants. Measure the psychosocial status of the elderly using the Indonesian version of the Self Reporting Questionnaire (SRQ) and the quality of life using the Indonesian version of the World Health Organization Quality of Life-Old (WHOQOL – OLD) questionnaire.
Results: Most elderly have a good quality of life, as many as 229 (65.1%), while a poor quality of life, as many as 30 people (8.5%). In the psychosocial variables, most respondents did not experience mental health disorders, as many as 260 people (74.1%). The Mann-Whitney test showed a significant relationship between Quality of Life and Psychosocial Status, in particular we obserbed in subjects without mental disorders in comparison to subjects with mental disorders a better quality of life, i.e. the elderly who do not suffer from mental disorders will show a tendency for a good quality of life.
Conclusions: Psychosocial status related to quality of life in the elderly with osteoarthritis during the Covid-19 pandemic. The elderly who do not suffer from mental disorders will show a tendency for a good quality of life.
Keywords: Elderly; Covid-19; Psychosocial; Quality of life
INTRODUCTION
Qualified elderly are elderly who, through the aging process, remain healthy and optimal physically, socially, and mentally to remain prosperous throughout life and participate in improving the quality of life as members of society [1,2]—osteoarthritis in the elderly results in limitations in carrying out daily activities independently. A study revealed that 2.6% of the elderly experienced total dependence, 1.2% with moderate support, and 96.3% with mild reliance [3]. Dependence, coupled with lifestyle changes, is one of the factors causing stress in the elderly [4,5].
The elderly with osteoarthritis who experience stress tend to experience sadness, and the body becomes weak, with reduced appetite and interest in all things [6,7]. As a result, they will experience delays in treatment, especially in the second year of the Covid-19 pandemic, where there is a statistical increase in cases in various parts of the world, including some areas in Indonesia, where the elderly are a group that is vulnerable to infection. The number of deaths continues to increase, especially in the elderly group [8–10]. If this condition is allowed to drag on, it will trigger depression. In addition, the elderly will find it difficult to motivate themselves to recover. The adaptation process that must undertake to all the changes experienced makes the elderly vulnerable to psychological disorders such as unstable emotional conditions, depression, or anxiety, and it may reduce the quality of life of the elderly [11,12].
Crisis in the elderly can be expressed as a condition of psychosocial disorders with characteristics including dependence on others, isolating themselves, or withdrawing from social activities for various reasons. The reasons include undergoing retirement, severe and prolonged illness, the death of a spouse, and undergoing health protocols during the Covid-19 period, where everyone must keep their distance and isolate themselves [6,13]. For the elderly, changing roles in the family, socio-economic, and social community resulted in setbacks in adapting to the new environment and interacting with the social environment [11,14].
Quality of life is a strategic issue that reflects the condition of the elderly in enjoying the rest of their life and preparing to die peacefully. Therefore, factors affecting the quality of life of the elderly should be accommodated by the elderly, families, and health providers [15,16]. One of the health service providers on the first line is the Public Health Center (PHC). PHC as a health service provider and acting as a center for community health development in its working area should develop health programs based on problems that develop in the community [17,18].
Psychological factors, as assessed by the Geriatric Depression Scale, and sociodemographic characteristics, such as marital status, income and leisure activities, had an impact on quality of life [19]. Other studies show that apart from social demographic factors, social organization and social support affect the quality of life of the elderly [20], and the ability to perform daily routine activities is the strongest predictor [21]. In addition to the aforementioned factors, it is necessary to explore the effects of the psychosocial status of the elderly during the Covid-19 pandemic because the elderly are prone to depression. Preliminary research shows an increase in depression, post-traumatic anxiety, and adjustment disorders in the elderly, and the risk of suicide increases sharply. Stress can also lower the body’s immunity, worsening the condition of the elderly who are already physically weak. Patients with a previous psychiatric disorder will tend to experience worsening [3,20].
The elderly group is very vulnerable to contracting Covid-19, plus declining physical health conditions are increasingly impacting the decline in the quality of life of the elderly, increasing mortality rates in the elderly group. For this reason, it is necessary to survey psychosocial health status, response, and quality of life during the Covid-19 pandemic. This study explores the psychosocial problems of the elderly with osteoarthritis during the Covid-19 pandemic.
MATERIALS AND METHODS
Study design
The type of research is analytic observational using the research design is cross sectional study.
Study Population
This study was conducted at the Jambi Nursing Home involving 351 randomly selected participants with the following sample criteria including age 55 years, living in Jambi Nursing Home for at least one year.
Instruments
Psychosocial status was measured using the Indonesian version of the Self-Reporting Questionnaire (SRQ), which consisted of 29 questions about the respondent’s condition during the last 30 days [21]. The Indonesian version of the SRQ-20 has 5 dimensions, namely energy, cognitive, depression, physiology, and anxiety. The YES answers to items 1 to 20 (symptoms of neurosis) indicated a psychological problem, and item number 21 meant using a psychoactive substance. One YES answer from items 22 to 24 (psychotic symptoms) indicates a severe problem and needs further treatment. One YES answer to items 25-29 indicates the presence of symptoms of PTSD (Post Traumatic Stress Disorder).
Psychosocial status was categorized into suffering and not suffering from mental disorders. A mental disorder is declared if at least 5 neurotic symptoms are found or there is at least 1 psychotic or PTSD (Post Traumatic Stress Disorder) symptom on the Self-Reporting Questionnaire (SRQ). Meanwhile, it is declared not suffering from mental disorders if there are only 4 items of neurotic symptoms and there are no psychotic symptoms or PTSD (Post Traumatic Stress Disorder) symptom on the Self-Reporting Questionnaire (SRQ). The variable “Psychosocial status” assigning the scores: 1 = suffering and 0 = not suffering for mental disorders.
Measurement of quality of life used the Indonesian version of the World Health Organization Quality of Life-Old (WHOQOL – OLD) questionnaire, which contains the respondents’ living conditions in the last four weeks consisting of 26 questions [22]. The variable “Quality of Life”, assigning the scores: 1 = poor, 2= moderate, 3 = good, and 4 = very good for each subject.
The Indonesian version of the World Health Organization Quality of Life-Old (WHOQOL – OLD) questionnaire consists of the Herth Hope Index, Perceived Social Support from Friends (PSS-Fr), Perceived Social Support from Family (PSS-Fa) [22]. The Indonesian version of the WHOQOL-BREFF questionnaire has been tested for validity and reliability by Priastana et al. [22] with a rcount value (0.361) and a Cronbach Alpha value = 0.965, so researchers do not need to test the validity and reliability again.
Sample size
The number of samples involved was 351 participants who were randomly selected from the population. Calculating the number of samples is determined using the Slovin formula [23], where from 2.880 people in the population, d = 0.05, the number of samples is 351.
Ethical Consideration
No economic incentives were offered or provided for participation in this study. The study protocol matched the Declaration of Helsinki ethical guidelines for clinical studies. This research has been approved by the Health Research Ethics Commission of the Health Polytechnic of the Jambi Ministry of Health with the number LB.02.06/2/111/2022.
Statistical analysis
Data are presented as number and percentage for categorical variables, and continuous data expressed as the mean ± standard deviation (SD) or median with Interquartile Range (IQR). The results of data normality analysis using the Kolmogorov Smirnov test showed that the data were not normally distributed. We found the relationship between Quality of Life and Mental disorders using the Mann–Whitney test (ordinal data vs dichotomous).
We considered all tests with P-value< 0.05 as significant. The statistical analysis was performed by SPSS software version 16.0.
RESULTS
The distribution of the characteristics of the research respondents is presented in table 1.

Table 1. Distribution of the Respondents characteristics
Table 1 show that most respondents were 55-64 years, as many as 186 (53%). Most sexes are male, with as many as 225 (64.1%) respondents. Most respondents had a high school education, with 227 (64.7%).
Table 2 shows that most elderly have a good quality of life, as many as 229 (65.1%), while a poor quality of life, as many as 30 people (8.5%).
In the psychosocial variables, most respondents did not experience mental health disorders, as many as 260 people (74.1%).
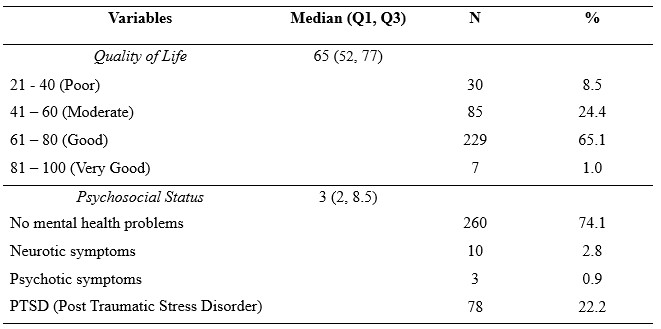
Table 2. Distribution of study variables
Table 3 shows that of the 91 respondents who do have mental disorders, there are 46 respondents with a moderate quality of life category. Of the 260 respondents with not mental disorders, there are 218 respondents have a good quality of life category
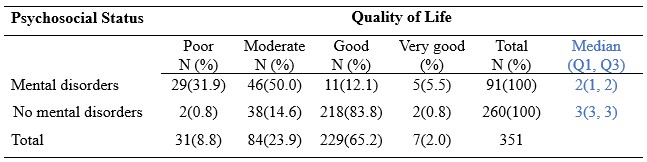
Table 3. Relationship between Psychosocial Status and Quality of Life in the Elderly
The Mann-Whitney test showed a significant relationship between Quality of Life and Psychosocial Status, in particular we obserbed in subjects without mental disorders in comparison to subjects with mental disorders a better quality of life (median: 3 vs 2, p<0.0001), i.e. the elderly who do not suffer from mental disorders will show a tendency for a good quality of life.
DISCUSSION
Elderly stress arises from anxiety about various diseases, including Covid-19. The current study aims to analyze the relationship between psychosocial conditions and the quality of life of the elderly with osteoarthritis during the Covid-19 pandemic.
The results of this study reported that on the psychosocial variables of the elderly, most of the elderly did not experience mental health disorders, as many as 260 people (74.1%) and the elderly and around 25.9% of the elderly experienced mental disorders ranging from PTSD (Post Traumatic Stress Disorder), neurotic and psychotic. Mental disorders experienced by the elderly include the elderly avoiding interacting with other people, decreasing interest in routine activities, always remembering the impact of Covid-19 and feeling disturbed, lack of appetite, not sleeping well, and feeling anxious. Symptoms of this health disorder significantly interfere with the quality of life of the elderly [24].
Anxiety, as a symptom of stress in the elderly in the Covid-19 pandemic situation, should receive support from spouses and family members by being willing to listen to the complaints of the elderly, being able and having time always to be near and accompany the elderly. Elderly family members are also responsible and act as friends of the elderly in dealing with their day-to-day. Likewise, in elderly stress, there is family support to maintain health by supporting the health of the elderly [25].
The increasing number of Covid-19 cases harms everyone’s mentality, especially the elderly. SARS-CoV-2 is highly contagious. Even some cases develop into respiratory failure, which will progress to death. Deterioration of the patient’s condition is more common in the elderly and those with previous co morbidities (hypertension, diabetes, heart disease) [26,27]. The elderly group (elderly) has physical and psychological weaknesses during the Covid-19 pandemic. About 20% of deaths with Covid-19 in China are over 60 years old [28].
The effects of quarantine are loneliness, sadness, and prolonged stress. Preliminary research suggests an increase in depression, post-traumatic stress, adjustment disorders in the elderly, and the risk of suicide [29]. Stress lowers immunity. This situation can worsen the condition of the elderly, who are already physically weak. Patients with previous psychiatric conditions will tend to experience worsening, one of which is the problem of osteoarthritis [30].
The main problem often experienced by the elderly with osteoarthritis is joint pain. Pain will increase when doing activities, which limits a person’s activities. The decrease in physical activity will affect the patient’s daily life activities and the quality of his life. A further consequence of osteoarthritis is decreased functional activity, especially difficulty rising to a sitting position, walking, and going up and down stairs [31,32]. The elderly with osteoarthritis will experience joint and muscle dysfunction, so they will experience limited movement, decreased strength, and muscle balance. About 18% experience difficulties and limitations in activities, loss of function of work capacity, and decreased quality of life [33,34].
According to Hong’s study [35], the elderly with osteoarthritis have a poorer quality of life than the elderly without osteoarthritis. This condition is associated with decreased physical function due to joint inflammation caused by joint damage. Therefore, it is highly recommended that families take care of the mental health of the elderly during Covid-19 so that it does not affect their physical health. Maintaining the mental health of the elderly during the Covid-19 pandemic requires assistance from all parties. Families, health workers, the government, and the elderly must cooperate. In addition, the knowledge, attitude, and behavior of the elderly need to be improved to deal with the Covid-19 pandemic. Adaptation and survival are the keys to overcoming this pandemic condition [29].
The primary strategy is to ensure that the elderly always maintain physical distance, wash their hands, use masks, eat nutritious foods, and do light exercise [36,37]. Other activities that can be done indoors, such as reading books, painting, or watching movies, can still be done. Explanations should be given as concisely as possible to the elderly. If the elderly understand, they will feel safe and peaceful and improve their quality of life. Social relations with family and friends must still be carried out through communication tools. Emotional support is crucial for the elderly who live alone. They are prone to anxiety and confusion during this uncertain period [9,38].
Visits to the doctor should be replaced with telemedicine. Patients can consult via Whatsapp, telephone, short message, Zoom, or any application. All planned surgeries should be postponed, such as cataracts, hernias, and kneecap replacements [38]. Any redundant information about Covid-19 should be reduced to prevent panic and misunderstanding. Information should focus on preventive measures, not on myths alone. Health information, updates about Covid-19, and psychological consultations should be provided by telephone or online by the government [30,39]. Although the elderly may appear weak from the outside, the family must try to give them a sense of freedom, respect, and genuine care. The elderly must still be involved in decision-making [40].
The World Health Organization (WHO) emphasizes the importance of psychosocial needs for the elderly [38]. The government is expected to provide basic needs for the elderly, especially those less well off financially and psychologically. The items that is important to prepare including food, medicines, and disinfectants. The need for security is essential and should not be ignored [41].
The strength of this study is that the two questionnaires used, namely the Self Reporting Questionnaire (SRQ) and the World Health Organization Quality of Life-Old (WHOQOL – OLD) questionnaire, have used the Indonesian version of the questionnaire to reduce research bias.
CONCLUSION
Psychosocial status related to quality of life in the elderly with osteoarthritis during the Covid-19 pandemic. The elderly who do not suffer from mental disorders will show a tendency for a good quality of life.
LIMITATIONS
The research location only involves 1 place so that it cannot compare the results of similar studies in different populations, so in the future research must be carried out involving several regions. Another limitation is the cross-sectional research design because it only measures the current condition of the variables, so it can cause research results to be biased.
FUNDING STATEMENT
This research did not receive any specific grant from funding agencies in the public, commercial, or not for profit sectors.
COMPETING INTERESTS STATEMENT
There are no competing interests for this study.
AUTHORS’ CONTRIBUTION
All authors equally contributed to preparing this article.
REFERENCES
- do Nascimento RJ, Barbosa Filho VC, Rech CR, Brasil RB, Junior RC, Streit IA, et al. Changes in Health-Related Quality of Life and Physical Activity Among Older Adults in the First-Wave COVID-19 Outbreak: A Longitudinal Analysis. Journal of Aging and Physical Activity. 2021;30(3):389–96.
- Ragni E, Mangiavini L, Viganò M, Brini AT, Peretti GM, Banfi G, et al. Management of Osteoarthritis During the COVID‐19 Pandemic. Clinical Pharmacology & Therapeutics. 2020;108(4):719–29.
- Pramono YS, Yuniarti Y, Anggraini L. Hubungan Derajat Insomnia Dengan Pemenuhan Kebutuhan Activity Of Daily Living Pada Lansia Di Panti Sosial Budi Sejahtera Banjarbaru 2019. Dinamika Kesehatan: Jurnal Kebidanan dan Keperawatan. 2019;10(2):916–27.
- Lábadi B, Arató N, Budai T, Inhóf O, Stecina DT, Sík A, et al. Psychological well-being and coping strategies of elderly people during the COVID-19 pandemic in Hungary. Aging & Mental Health. 2022;26(3):570–7.
- Nimitha KJ, Singh B, Srivastava RN, Kumar R. SYMPOSIUM Health Related Quality Of Life And Depression In Older Adults With Knee Osteoarthritis Pain-Cross-Sectional Telephonic Survey In Covid 19 Pandemic. Indian journal of psychiatry. 2022;64(Suppl 3):S634.
- Giacalone A, Rocco G, Ruberti E. Physical health and psychosocial considerations during the COVID-19 outbreak. Psychosomatics. 2020;61(6):851–2.
- Dubey S, Biswas P, Ghosh R, Chatterjee S, Dubey MJ, Chatterjee S, et al. Psychosocial impact of COVID-19. Diabetes & Metabolic Syndrome: clinical research & reviews. 2020;14(5):779–88.
- Onder G, Rezza G, Brusaferro S. Case-fatality rate and characteristics of patients dying in relation to COVID-19 in Italy. Jama. 2020;323(18):1775–6.
- Lee K, Jeong G-C, Yim J. Consideration of the psychological and mental health of the elderly during COVID-19: A theoretical review. International journal of environmental research and public health. 2020;17(21):8098.
- Akat M, Karataş K. Psychological effects of COVID-19 pandemic on society and its reflections on education. Electronic Turkish Studies. 2020;15(4).
- Min Fui W, Abdul Majid H, Ismail R, Su TT, Maw Pin T, Said MA. Psychosocial factors associated with mental health and quality of life during the COVID-19 pandemic among low-income urban dwellers in Peninsular Malaysia. PloS one. 2022;17(8):e0264886.
- Bidzan-Bluma I, Bidzan M, Jurek P, Bidzan L, Knietzsch J, Stueck M, et al. A Polish and German population study of quality of life, well-being, and life satisfaction in older adults during the COVID-19 pandemic. Frontiers in psychiatry. 2020;11:585813.
- Wiraini TP, Zukhra RM, Hasneli Y. Hubungan Dukungan Keluarga Dengan Kualitas Hidup Lansia Pada Masa COVID-19. Health Care: Jurnal Kesehatan. 2021;10(1):44–53.
- Muliani R, Jayanti TN, Dirgahayu I, Safarudin I, Anri A. Psychosocial Support in Increasing COVID-19 and Mental Health in The Elderly. JCES (Journal of Character Education Society). 2021;4(1):135–47.
- Zulka AN, Suryaningsih Y, Wulandari PNM, Putri DA. Evaluasi Manajemen Penyakit dan Psychological Well Being Lansia di Masa Pandemi Covid 19. The Indonesian Journal of Health Science. 2022;14(1):84–91.
- Juwita R. Meningkatkan Kualitas Hidup Lansia Pasca Pandemi Covid 19. Jurnal Mitra Prima. 2022;4(2).
- Rayani D, Purqoti DNS. Kecemasan Keluarga Lansia Terhadap Berita Hoax Dimasa Pandemi COVID-19. Realita: Jurnal Bimbingan dan Konseling. 2020;5(1).
- Syahruddin S. Kebugaran Jasmani Bagi Lansia Saat Pandemi Covid-19. JUARA: Jurnal Olahraga. 2020;5(2):232–9.
- Alexandre T da S, Cordeiro RC, Ramos LR. Factors associated to quality of life in active elderly. Revista de saude publica. 2009;43:613–21.
- Guida C, Carpentieri G. Quality of life in the urban environment and primary health services for the elderly during the Covid-19 pandemic: An application to the city of Milan (Italy). Cities. 2021;110:103038.
- Idaiani S, Suryaputri IY, Mubasyiroh R, Indrawati L, Darmayanti I. Validity of the Self Reporting Questionnaire-20 for Depression Based on National Health Survey. 2021;
- Priastana IKA, Kusumaningtiyas DPH. Quality of Life in The Elderly Viewed from Hope, Friend Support, and Family Support. STRADA Jurnal Ilmiah Kesehatan. 2020;9(2):1670–5.
- Sugiyono. Metode penelitian pendidikan pendekatan kuantitatif, kualitatif dan R&D. Alfabeta; 2013.
- Widyaningrum DA, Umam FN. Pengaruh Nyeri Sendi Terhadap Kualitas Tidur dan Kualitas Hidup Pada Lansia Penderita Osteoartritis. Jurnal Keperawatan. 2020;13(2):7.
- Intarti WD, Savitri NPH. Manfaat Relaksasi Yoga Dan Swedish Massage Terhadap Stress Lansia Saat Pandemi Covid-19. Jurnal Bina Cipta Husada. 2021;17(1):96–112.
- Banerjee D. ‘Age and ageism in COVID-19’: Elderly mental health-care vulnerabilities and needs. Asian journal of psychiatry. 2020;51:102154.
- Jing Z, Li J, Wang Y, Ding L, Tang X, Feng Y, et al. The mediating effect of psychological distress on cognitive function and physical frailty among the elderly: evidence from rural Shandong, China. Journal of affective disorders. 2020;268:88–94.
- Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention. jama. 2020;323(13):1239–42.
- Perrotta F, Corbi G, Mazzeo G, Boccia M, Aronne L, D’Agnano V, et al. COVID-19 and the elderly: insights into pathogenesis and clinical decision-making. Aging clinical and experimental research. 2020;32(8):1599–608.
- Armitage R, Nellums LB. COVID-19 and the consequences of isolating the elderly. The Lancet Public Health. 2020;5(5):e256.
- Peat G, McCarney R, Croft P. Knee pain and osteoarthritis in older adults: a review of community burden and current use of primary health care. Annals of the rheumatic diseases. 2001;60(2):91–7.
- Jakobsson ULF, Hallberg IR. Pain and quality of life among older people with rheumatoid arthritis and/or osteoarthritis: a literature review. Journal of clinical nursing. 2002;11(4):430–43.
- Neogi T. The epidemiology and impact of pain in osteoarthritis. Osteoarthritis and cartilage. 2013;21(9):1145–53.
- McCaffrey R, Freeman E. Effect of music on chronic osteoarthritis pain in older people. Journal of advanced nursing. 2003;44(5):517–24.
- Hong J-Y, Han K, Shin D-H, Chun EM. Quality of life analysis and smoking correlation in symptomatic spine osteoarthritis: a nationwide health survey analysis of an elderly population with EQ-5D. PLoS One. 2016;11(3):e0151315.
- Meng H, Xu Y, Dai J, Zhang Y, Liu B, Yang H. Analyze the psychological impact of COVID-19 among the elderly population in China and make corresponding suggestions. Psychiatry research. 2020;289:112983.
- Girdhar R, Srivastava V, Sethi S. Managing mental health issues among elderly during COVID-19 pandemic. Journal of geriatric care and research. 2020;7(1):32–5.
- Banerjee D. The impact of Covid‐19 pandemic on elderly mental health. International journal of geriatric psychiatry. 2020;35(12):1466.
- Petretto DR, Pili R. Ageing and COVID-19: what is the role for elderly people? Vol. 5, Geriatrics. MDPI; 2020. p. 25.
- Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: A comparison with young and middle-aged patients. Journal of Infection. 2020;80(6):e14–8.
- Papadopoulos V, Li L, Samplaski M. Why does COVID‐19 kill more elderly men than women? Is there a role for testosterone? Andrology. 2021;9(1):65–72.
![]() This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.

